RAC: It's Big and Getting Bigger
CMS Awards Contracts for Permanent National RAC Program
Fueled by the collection of more than $900 million in overpayments and the return of almost $38 million in underpayments, Medicare is rolling out the permanent Recovery Audit Contractor (RAC) program. On October 6, Medicare released the names and RAC jurisdictions as follows:
- HealthDataInsights, Inc. of Las Vegas, Nevada: REGION D (encompassing Montana, Wyoming, North Dakota, South Dakota, Utah, Arizona, Washington, California, Oregon, Idaho, Nevada, Nebraska, Kansas, Iowa, Missouri, Hawaii, and Alaska)
- Diversified Collection Services, Inc. of Livermore, California: REGION A (encompassing Rhode Island, New Hampshire, Vermont, Massachusetts, Delaware, Connecticut, New York, Pennsylvania, New Jersey, and Maine)
- CGI Technologies and Solutions, Inc. of Fairfax, Virginia: REGION B (encompassing Minnesota, Michigan, Wisconsin, Indiana, Illinois, Kentucky, and Ohio)
- Connolly Consulting Associates, Inc. of Wilton, Connecticut: REGION C (encompassing South Carolina, North Carolina, Florida, Colorado, New Mexico, Texas, Oklahoma, Alabama, Tennessee, Georgia, Mississippi, West Virginia, Virginia, Louisiana, and Arkansas)
In the RAC demonstration project, Connolly Consulting and HealthDataInsights were Claims RACs and Diversified Collection Services was a Medicare Secondary Payer RAC.
Background
The Medicare Modernization Act (MMA) of 2003 directed CMS to conduct a three-year demonstration program focused on recovery audits in a handful of states, principally California, New York, and Florida. Commenced in 2005, the program's mission was to reduce improper payments, detect and collect overpayments, identify underpayments, and implement systems to prevent future improper payments, but not to review claims that had already been reviewed by fiscal intermediaries, carriers, or other governmental agents. CMS overall was pleased with the program's results, touting a “respectable return on investment” from RAC audits of well over 300 percent.
Providers in states subject to RAC audits complained of the bias inherent in paying RACs on a contingency-fee basis, which even CMS admitted resulted in a focus on high dollar improper payments (e.g., inpatient hospital claims) to give the highest return relative to the cost of reviewing claims and medical records. And while RACs are required to use the same Medicare policies used by fiscal intermediaries, carriers, and other government agents, providers complained about the RACs apparent inexperience with such policies, the lack of physicians and certified coders on RAC staff, and the burdensome and unfettered methods used by RACs to request medical records.
Additionally, providers complained about, and appealed, RAC denials that concerned claims paid more than three years prior to the RAC's denials, without a showing of good cause for such late reopenings. Such appeals were frequently successful at the third-appeals level before Administrative Law Judges (ALJs), but recent appeals have been overturned at the fourth-appeals level before the Medicare Appeals Council, on the grounds that ALJs lack jurisdiction to review that issue. Whether the Medicare Appeals Council's stance survives further challenges remains to be seen.
Permanent RAC Program
Any provider or supplier that bills Medicare Parts A and B is subject to a RAC audit, including hospitals, physician practices, nursing homes, home health agencies, and durable medical equipment suppliers. Each RAC will have exclusive jurisdiction in its assigned Region for the RAC audits of Medicare fee-for-service claims that have not otherwise been reviewed by other Medicare contractors for improper payments. Improper payments may be overpayments or underpayments.
Significantly for providers, Permanent RACs will continue to be paid on a contingency fee basis on both the overpayments and underpayments. But, CMS has extensively revised the RAC program in an attempt to resolve complaints and other issues that arose in the RAC demonstration project. The primary changes are reflected in the CMS chart below:
Table 10. Improvements Made to the RAC Permanent Program
| Issue | Demonstration RACs | Permanent RACs |
| RAC medical director | Not Required | Mandatory |
| Coding experts | Optional | Mandatory |
| Credentials of reviewers provided upon request | Not Required | Mandatory |
| Discussion with CMD regarding claim denials if requested | Not Required | Mandatory |
| Minimum claim amount | $10.00 aggregate claims | $10.00 minimal claims |
| AC validation process | Optional | Limited |
| External validation process | Not Required | Mandatory |
| RAC must payback the contingency fee if the claim is overturned on appeal | Only required to pay back if claim is overturned on the first level of appeals | Required to pay back if claim is overturned at all levels of appeals |
| Vulnerability reporting | Limited | Frequent and mandatory |
| Standardized base notification of overpayment letters to providers | Not Required | Mandatory |
| Look back period (from claim pmt date - date of medical record request) | 4 years | 3 years |
| Maximum look back date | None | 10/1/2007 |
| Allowed to review claims in current fiscal year? | No | Yes |
| Limits on # of medical records requested | Optional. Each RAC set own limit | Mandatory. CMS will establish uniform limits |
| Time frame for paying hospital medical record photocopying vouchers | None | Within 45 days of receipt of medical record |
| MSP included | Yes | No |
| Quality assurance/Internal control audit | No | Mandatory |
| Remote call monitoring | Yes | Yes |
| Reason for review listed on request for records letters and overpayment letters | Not Required | Mandatory |
| RAC claim status Web page | Not Required | By January 2010 |
| Public disclosure of RAC contingency fees | No | Yes |
| The Medicare RAC Demonstration | ||
What To Expect
During the next two months, look for your permanent RACs to hold town hall meetings to educate and inform providers in your area. The following schedule highlights the roll-out in each jurisdiction:
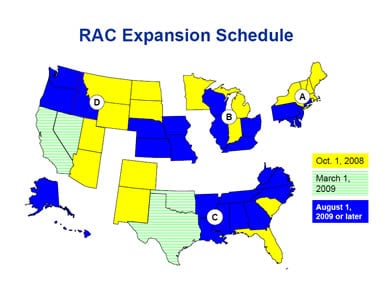
The nationwide rollout will be completed by Jan. 1, 2010. The nationwide rollout will be completed by Jan. 1, 2010.
What Actions Can You Take Now?
We recommend that you begin efforts now to prepare for the Permanent RAC Program. These efforts include assessing the completeness of medical records, reviewing and assessing compliance with coverage and coding requirements, and familiarizing yourself with RAC procedures and appeal deadlines. Providers that take these steps will be able to:
- Respond faster and with less expense to RAC requests
- Reduce the number of RAC denials
- Avoid missed appeal deadlines
We recommend that you pay close attention to RAC denials. The administrative appeal process available for contesting RAC denials has strict timelines and requires you to submit all supporting documentation early in the appeal process. As a result, you may wish to consult with legal counsel at an early stage of any RAC denial
